September 2022 Case Study
by Alexis Carrington, MD
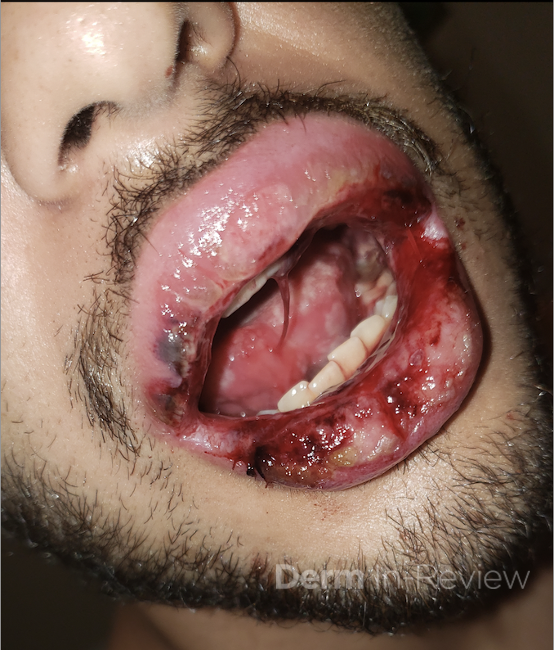
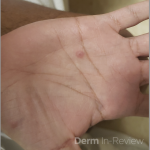
A 22 year-old male with a past medical history of asthma presents to the ED with a rash on the mouth and bilateral palms that appeared a day prior to presentation. A week prior, he went to the ED for worsening throat and mouth pain, where he was diagnosed with thrush and given nystatin but didn’t have any skin manifestations at that time. He also reported subjective fevers, chills, decreased appetite, fatigue and non-bloody diarrhea that started two days ago. Exam showed hemorrhagic mucositis with some minor re-epithelialization and a papular target lesions on the hands and left arm. Based on examination, a diagnosis of Erythema Multiforme was made.
What is the most common precipitating factor for Erythema Multiforme?
A.) Herpes Simplex Virus (HSV)
B.) Parapoxvirus
C.) Mycoplasma pneumoniae
D.) Histoplasma capsulatum
Correct answer: A.) Herpes Simplex Virus (HSV)
Erythema Multiforme (EM) is an immune-mediated mucocutaneous condition characterized by “target” lesions. Severe mucosal involvement is what distinguishes erythema multiforme major from erythema multiforme minor. EM episodes can be recurrent or persistent, but are typically self-limiting. Some triggers of EM include infections, as well as medications and even vaccinations.
The characteristic morphology of EM are typical target lesions, which are a round shape with a well defined border and consist of three distinct zones distributed on the extremities and the face, the dorsal hands and forearms being the most frequently involved. Mucosal lesions of EM are vesiculobullous and develop into painful erosions on the buccal mucosa and lips. Diagnosis is clinical but not based solely on histological findings.
The most common associated infectious agent with EM is Herpes Simplex Virus (answer A). Parapoxvirus (answer B) Histoplasma capsulatum (answer D) and Mycoplasma pneumoniae (answer C) are observed less frequently.
Treatment is supportive as EM episodes are typically self limiting. However, early therapy with systemic corticosteroids can be considered in severe forms of EM with functional impairment.
References
- Canavan TN, Mathes EF, Frieden I, Shinkai K. Mycoplasma pneumoniae-induced rash and mucositis as a syndrome distinct from Stevens-Johnson syndrome and erythema multiforme: a systematic review. J Am Acad Dermatol. 2015;72(2):239–45. doi:10.1016/j.jaad.2014.06.026.
- Soares A, Sokumbi O. Recent Updates in the Treatment of Erythema Multiforme. Medicina (Kaunas). 2021;57(9):921. Published 2021 Sep 1. doi:10.3390/medicina57090921.
- Bolognia, Jean L. Dermatology volume 2. Mosby, 2018.