July 2022 Case Study
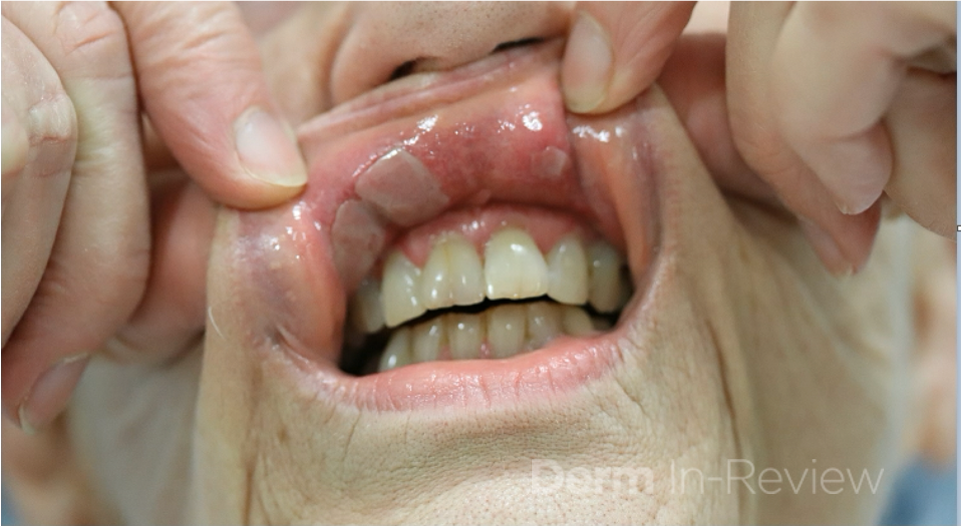
A 70-year-old woman with history of hypothyroidism and asthma presents to clinic with a 3-month history of sores in her mouth. She denies any other symptoms, but she does report a 5-pound weight loss due to pain with eating. On further exam, there are erosions of the gingiva, buccal mucosa, and posterior neck. There is no involvement of other mucosal sites. Patient undergoes biopsies for hematoxylin and eosin staining and direct immunofluorescence (DIF). Results showed a subepidermal bullae with positive IgG and C3 staining at the dermo-epidermal junction. Further testing revealed presence of anti-laminin 332 antibodies.
What additional work up is needed?
A.) Referral to ophthalmology
B.) Pulmonary function testing
C.) Perform all age-appropriate cancer screenings
D.) Endoscopy
E.) No additional work up needed
Correct answer: C.) Perform all age-appropriate cancer screenings
Mucous membrane pemphigoid (MMP) is a subepidermal autoimmune blistering disorder with various phenotypes. As the name suggests, clinical features involve erosions of mucosal surfaces, often with subsequent scarring. The most commonly affected mucosal sites are oral and ocular surfaces. Those with ocular involvement are at risk for blindness so it is important to ensure ophthalmologic monitoring when necessary. Non-mucosal skin can be affected, but this occurs in less than 50% of patients.1
Previously, subtypes were classified based on antigenic targets or area of involvement – anti-elipigrin cicatricial MMP (laminin 332), ocular MMP (b4 subunit of integrin a6b4), anti-bullous pemphigoid antigen MMP (BPAG180 or BPAG230).1 Additionally, the “Brunsting-Perry” variant classified a subset of patients with cutaneous involvement of the head and neck resulting in a cicatricial alopecia.1 However, recent updates in nomenclature have moved away from use of these subtypes and toward use of phenotypic descriptions.2
Diagnosis of MMP requires a combined approach as diagnosis can often be delayed. As with other vesiculobullous diseases, DIF is essential to diagnosis and has been found to be the most sensitive diagnostic tool.3,4 Classic findings on DIF are IgG, IgA, and/or C3 deposition at the dermo-epidermal junction.4 Salt split skin technique is useful to differentiate likely antigenic targets. Roof staining with IgG or IgA is consistent with BP180 or BP230 targets while floor staining with IgG or IgA correlates to laminin 332 or type VII collagen targets.4 It is important to remember that anti-laminin 332 MMP, as seen in this patient, is associated with an increased risk of malignancy.1,4 Thus, it is important that patients with this variant undergo age-appropriate cancer screenings at the time of diagnosis.
References
- Bolognia JK, Schaffer JV, Cerroni L. Dermatology. Philadelphia: Elsevier. 2018.
- Rashid H, et al. European guidelines (S3) on diagnosis and management of mucous membrane pemphigoid, initiated by the European Acadmy of Dermatology and Venereology – Part I. 2021;35:1750-1764.
- Rashid H et al. Assessment of diagnostic strategy of mucous membrane pemphigoid. JAMA Derm. July 2021;157(7):780-787.
- Schmidt E, et al. European guidelines (S3) on diagnosis and management of mucous membrane pemphigoid, initiated by the European Academy of Dermatology and Venereology – Part II. JEADV. 2021;35:1926-1948.