April 2022 Case Study
by Blair Allais, MD
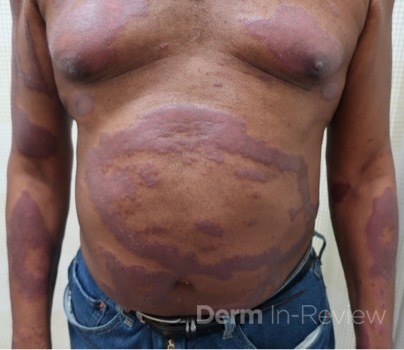
A 63-year-old male presented to clinic with a 2-year history of asymptomatic annular hypopigmented plaques on the trunk and extremities that eventually became erythematous to violaceous. He had been prescribed topical steroids by an outside practitioner without improvement in the lesions. Biopsy performed on one of the plaques revealed a granulomatous reaction surrounding adnexal structures and in the papillary dermis. Fite stain revealed numerous pink to red acid-fast organisms within the granulomas ultimately rendering a diagnosis of lepromatous leprosy. The patient was started on therapy with Rifampin 600mg monthly, Minocycline 100mg monthly and Moxifloxacin 400mg monthly. Approximately 3 months after initiating treatment the patient developed new nodular skin lesions on the extensor arms and medial thighs associated with fever, myalgias, fatigue and joint pain.
What is the best course of treatment for this patient’s new presentation?
A.) Prednisone
B.) Clofazimine
C.) Thalidomide
D.) Methotrexate
Correct answer: C) Thalidomide
The patient described has a diagnosis of lepromatous leprosy and is experiencing a reactional state to treatment. Approximately 50% of patients with leprosy will experience a reaction after the institution of therapy. Aside from initiating antibiotic therapy, other causes of reactional states include intercurrent infections, vaccination, pregnancy, vitamin A, iodides and bromide. Reactions are an important cause of permanent nerve damage in borderline patients and are abrupt in appearance.
Two major types of reactional states have been described. Type 1 reactions due to enhancement of cell-mediated immunity with a Th1 cytokine pattern (IFN-y, TNF, IL-1ß, IL-2, IL-12). These reactions are considered to reversal reactions with “upgrading” and are seen predominantly in borderline or tuberculoid forms of leprosy. They are characterized by increased inflammation within existing skin lesions in addition to acute nerve pain or tenderness (neuritis) and loss of function. Treatment of choice for these reactions is prednisone (A) starting at a dose of 40 – 60 mg/day. Neuritis and eye lesions are urgent indications for therapy and dose and duration is determined by the clinical course of the reaction. Steroids are tapered slowly over months to years once the reaction is controlled. In some cases, clofazimine (B) may be added as it has some activity against the type 1 reaction, and may be added in doses of up to 300 mg/day as tolerated.
Type 2 reactions are due to excessive humoral immunity with a Th2 cytokine pattern (IL-4, IL-10) and characterized by formation of immune complexes. They are seen predominately in patients with lepromatous and borderline lepromatous forms of leprosy, especially in patients with a high bacterial load who are undergoing treatment. Multisystem involvement is seen with systemic symptoms including nodular skin lesions, fever, myalgias, malaise, severe joint swelling and pain, iridocyclitis, lymphadenitis, hepatosplenomegaly, orchitis and glomerulonephritis. The intensity of the reaction can vary from mild to severe and can last from a few days to weeks, months, or even years. Pathology is characterized by cutaneous and systemic small vessel vasculitis, and treatment of choice is Thalidomide (C). According to the newly developed U.S. regimen for treatment for lepromatous leprosy, methotrexate (D) 15mg weekly can be prescribed to prevent reactions at the time of initiating multi drug treatment.
References
- Ramos-e-Silva M, Ribeiro de Castro MC. Chapter 75: Mycobacterial Infections. 4th Ed. Philadelphia, PA: Elsevier; 2018.
- James WD et al. Chapter 17: Hansen Disease. Andrews’ Diseases of the Skin. 13th Philadelphia, PA: Elsevier; 2020.
- Bennett JE et al. Principles and Practice of Infectious Diseases. 6th edit.P.2887-2896