February 2026 Case Study
Caroline Clark, MD1
- Department of Dermatology, George Washington University School of Medicine and Health Sciences
Patient History
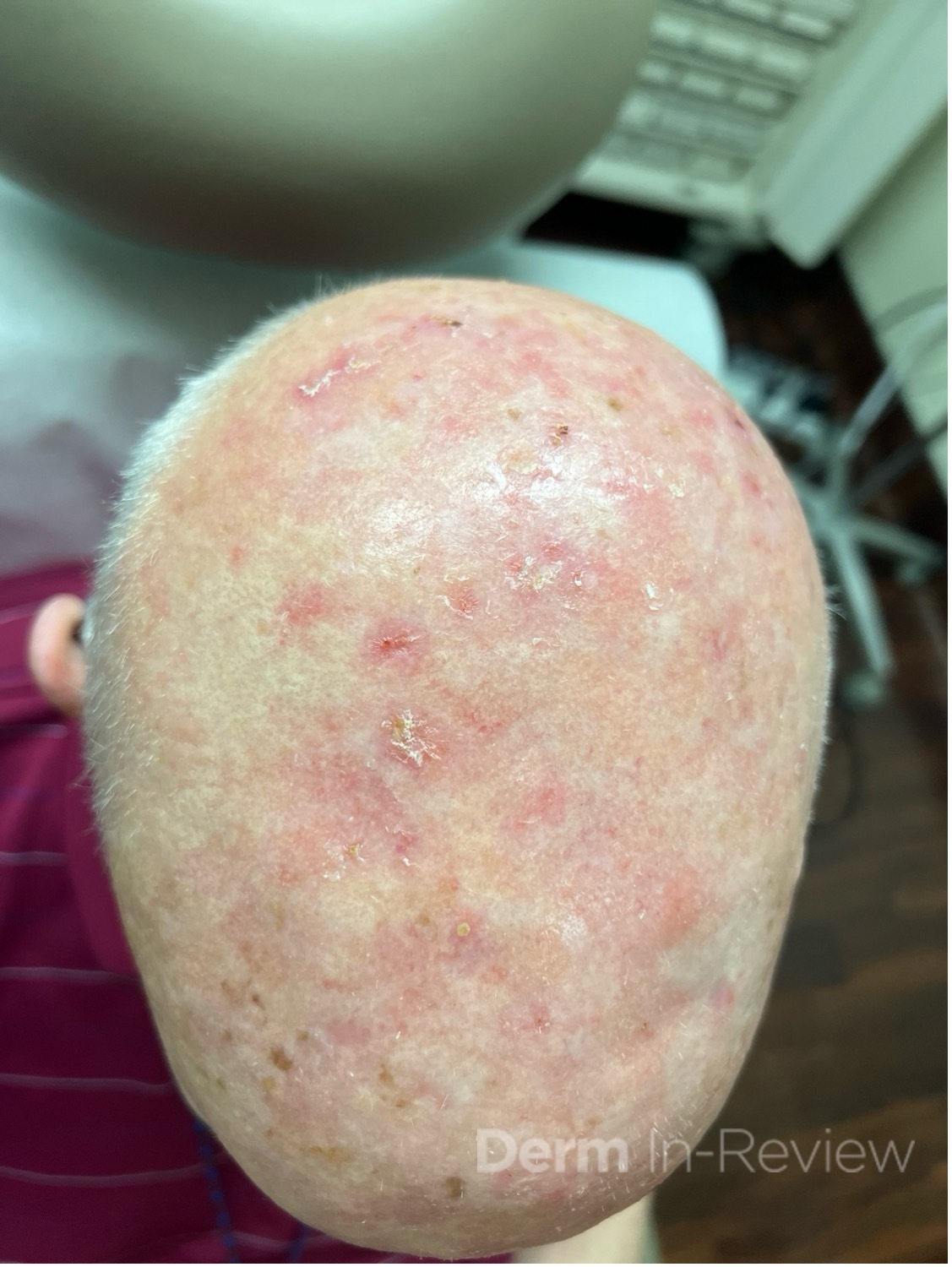
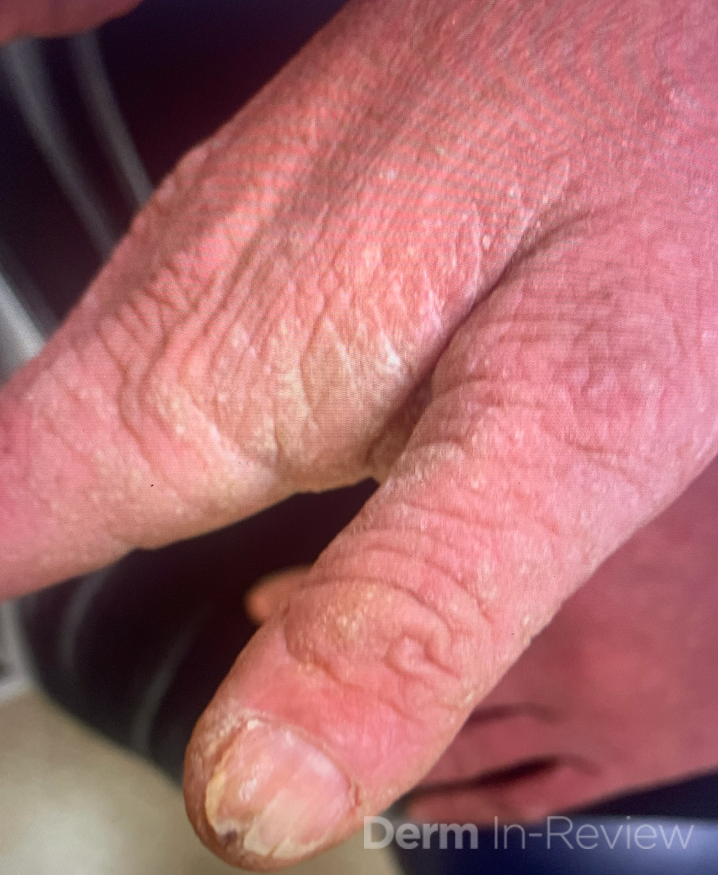
A 19-year-old woman presents to dermatology clinic with a 3-year history of a progressively worsening rash on her neck, chest and hands, and nail changes. The rash is mildly itchy, has a strong odor, and worsens during the summer months when she is sweating or spending time outdoors. She has tried over-the-counter acne treatments and moisturizers without improvement.
Her father reports having similar skin problems that began in his teenage years.
Laboratory studies including complete blood count, comprehensive metabolic panel, and thyroid function tests are within normal limits.

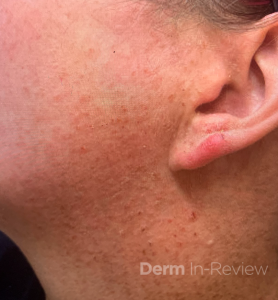
A gene mutation affecting which of the following processes is most likely responsible for this patient’s skin findings?
A) Keratinocyte proliferation and differentiation
B) Degradation of keratin through proteolytic enzymes
C) Keratinocyte Adhesion
D) Endoplasmic Reticulum calcium transport
E) Golgi Apparatus calcium transport
Correct Answer: D
Explanation/Literature Review
Darier disease is an autosomal dominant genodermatosis caused by mutations in the ATP2A2 gene, which encodes the sarco/endoplasmic reticulum (ER) calcium ATPase type 2 (SERCA2) pump (Answer choice D). This genetic defect impairs intracellular calcium homeostasis, leading to desmosome breakdown, acantholysis, and abnormal keratinization.1
The disease typically manifests in the second decade of life with greasy, yellow-brown keratotic papules and plaques in a seborrheic distribution (face, chest, back) and flexural regions, often accompanied by a characteristic malodor.1,2 Nearly all patients develop nail abnormalities including red and white longitudinal streaks with V-shaped notches at the distal edges, and many have palmoplantar pits and oral mucosal papules.
Histologically, the hallmark features are suprabasilar acantholysis with corps ronds (enlarged keratinocytes with fragmented nuclei in the spinous layer) and corps grains (small oval cells in the stratum corneum).2
The disease follows a chronic relapsing course with exacerbations triggered by heat, humidity, UV radiation, mechanical trauma, and infections.1,3
Treatment remains largely symptomatic, with oral retinoids being most effective for extensive disease, though recent evidence suggests targeting the IL-23/IL-17 axis may provide benefit in therapy-resistant cases.1,4
Explanation of Incorrect Answers
Keratinocyte adhesion (Answer choice C) is impaired in Darier disease due to ER stress and abnormal desmosome/adherens junction formation, but this is a downstream consequence rather than the primary molecular defect. Abnormal keratinocyte proliferation and differentiation (Answer choice A) are seen in psoriasis, which affects the nails with pitting, onycholysis, and subungual hyperkeratosis. The nail findings seen in onychomycosis are a result of the dermatophyte’s degradation of keratin through proteolytic enzymes (Answer choice B). Lastly, Hailey-Hailey disease (benign familial pemphigus) is caused by a mutation in ATP2C1 encoding SPCA1, a secretory pathway Ca²⁺-ATPase located in the Golgi apparatus (Answer choice D). Both Hailey-Hailey and Darier disease are calcium pump disorders with overlapping clinical features including acantholysis, however the keratotic papules and nail V-nicking are more characteristic of Darier disease.
References
- Ettinger M, Kimeswenger S, Deli I, Traxler J, Altrichter S, Noack P, Wikstrom JD, Guenova E, Hoetzenecker W. Darier disease: Current insights and challenges in pathogenesis and management. J Eur Acad Dermatol Venereol. 2025 May;39(5):942-951. doi: 10.1111/jdv.20448. Epub 2024 Nov 28. PMID: 39606894; PMCID: PMC12023721.
- Engin B, Kutlubay Z, Erkan E, Tüzün Y. Darier disease: A fold (intertriginous) dermatosis. Clin Dermatol. 2015 Jul-Aug;33(4):448-51. doi: 10.1016/j.clindermatol.2015.04.009. Epub 2015 Apr 9. PMID: 26051059.
- Atzmony L, Zagairy F, Mawassi B, et al. Persistent Cutaneous Lesions of Darier Disease and Second-Hit Somatic Variants in ATP2A2 Gene. JAMA Dermatol. 2024;160(5):518–524. doi:10.1001/jamadermatol.2024.0152
- Ettinger M, Burner T, Sharma A, Chang YT, Lackner A, Prompsy P, Deli IM, Traxler J, Wahl G, Altrichter S, Langer R, Tsai YC, Varkhande SR, Schoeftner LC, Iselin C, Gratz IK, Kimeswenger S, Guenova E, Hoetzenecker W. Th17-associated cytokines IL-17 and IL-23 in inflamed skin of Darier disease patients as potential therapeutic targets. Nat Commun. 2023 Nov 17;14(1):7470. doi: 10.1038/s41467-023-43210-5. PMID: 37978298; PMCID: PMC10656568.